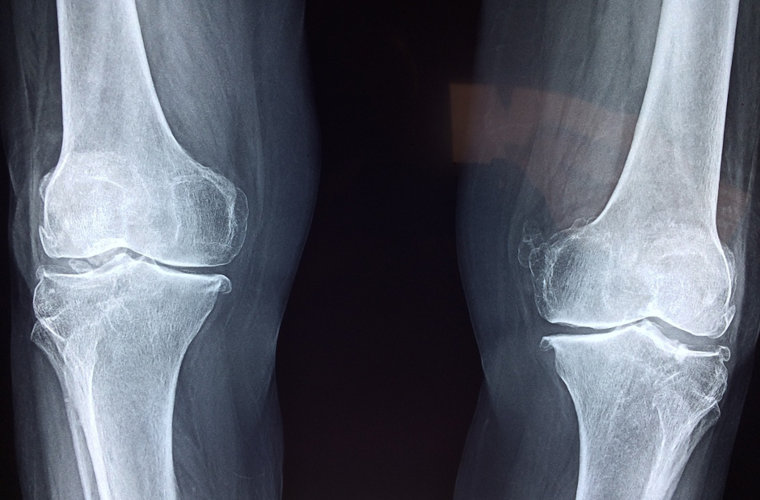
You have arthritis. What now?
The closed ended diagnosis of arthritis can feel like a death sentence:
- Wear and tear.
- Your joint surface is damaged.
- The damage is responsible for your pain.
- Using the joint will damage it more.
- You need to stop doing the activities you enjoy.
- You’ll be stuck on stomach and kidney-destroying medication which only take the edge off on some days until you fuse or replace the joint.
- Cortisone injections might help if they don’t cause more damage.
- Scraping the joint may buy you some time but the damage is done, and the joint replacement is inevitable.
Unless you’re looking for a reason to have an operation, please ignore the dooms-day inaccuracies above and continue reading… This is the perfect time to learn that surgeons are best geared to offer surgical solutions, but they aren’t that well versed in the alternatives to surgery because that’s simply not their job. The same goes for GPs, radiologists, your best friend and the internet. Its also not too late simply because your pain has been ongoing for years or because you picked up weight at some point in the past.
Be kind to yourself while considering the following:
- A diagnosis based on your symptoms and history alone is at best an easy guess.
- You’ll usually get different guesses from different people – whether they are qualified to have an opinion or not.
- Scans don’t tell the full story outside of traumatic injuries for musculoskeletal problems. Since we can’t see function on a scan, it already assumes pain must have a structural cause and any findings (even harmless ones) are incorrectly assigned to the cause of your symptoms.
- The good news is that we see bona fide arthritis in the totally asymptomatic population just as often as what we do in people in pain.
This doesn’t mean you don’t have arthritis, and it doesn’t mean that arthritis isn’t causing your pain, but it does mean that scans and x-rays are unreliable in determining the cause of your pain and if you believe the x-ray, you may be shacking yourself up with an irrelevant diagnosis while missing the solution to the symptoms plaguing you.
Clues to suggest that your “arthritis” may not be the cause of your pain:
- Relief with pressure: Even if this only happens occasionally
- Migrating pain: Shifts in where the joint hurts or which joint hurts
- Whole limb complaints: If the pain sometimes spreads to more joints in the same limb
- Unpredictable triggers: If a movement or position is problematic one day and not on another
- Pain escalating with rest: A palpable increase in the intensity of pain while you’re giving the joint a break for a few minutes / hours.
So, you may / may not necessarily have arthritis but, “What now?”
If surgery is something you’d like to avoid, then seeing someone who appreciates the mechanical, physiological and chemical environments in addition to the structure is essential – even if the surgeon said your joint is too far gone – pinch of salt, please. The inconsistencies mentioned above are typically observed in mechanical conditions (even when the structure seems to be a disaster). While consistency is possible in mechanical conditions, it is imperative for the diagnosis of structural conditions such as arthritis. Noting and understanding any inconsistencies is key in uncovering the real cause of pain for people with “arthritis”.
Your health and wellbeing deserves quality care. Make sure to discuss any concerns you may have directly with your preferred physiotherapist, so that you can receive the appropriate guidance for your unique situation.
Your health and wellbeing deserve informed, personalised care. For tailored support, please discuss any questions or concerns with your physiotherapist of choice.